Examples & Case Studies:
Several case studies (Upper limb, lower limb and spinal pathologies) are included below.
These are examples intended to illustrate how common musculoskeletal issues may be managed. Names and patient details have deliberately been changed to maintain patient confidentiality.
There are often various options for managing these conditions. Patients will have an individualised management plan tailored to their own needs and specific circumstances.
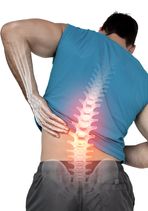
LOW BACK PAIN
Joe is a fit and active man who enjoys sports and lifting weights in the gym. He was previously a high-level athlete. He recently completed university and has started working at a deskjob, putting in long hours at work. He admits to a degree of stress and lack of rest.
He has suffered with low back pain for a few months. This has gradually become more frequent and intense. It is worse on the left side and is noted on waking up, improving as the day goes on. He finds it uncomfortable to stand for any period of time.
He attends for a clinic consultation. A detailed history and clinical examination is carried out. This includes a neurological examination.
An MRI scan of his lumbar spine (lower back) is arranged. This confirms the clinical suspicion of a facet syndrome at the left L4/5 and L5/S1 facet joints.
Blood tests are also carried out to exclude an inflammatory condition and are reported as completely normal.
Following discussion, Joe is started on oral painkillers and referred for osteopathic treatment.
Advice about sleep position, posture and avoiding typical activities that are likely to set the pain off are also addressed. Stress management strategies are interwoven into the discussion.
He is reviewed again after 2 months. He has noted some improvement but due to the repetitive nature of his office work, the problem continues to recur.
The option of CT-guided facet joint injections is discussed. He considers this and decides to proceed. He notices improvement almost immediately and is able to come off the oral painkillers.
He has an ergonomic assessment at work and also makes a concerted effort to take more regular breaks during the working day to hydrate and stretch out his back muscles.
The injury prevention aspect is discussed in greater detail and he decides to attend a once weekly Pilates reformer class to improve his lumbopelvic strength and stability.
Whenever Joe feels his back muscles start to tighten up as a result of long hours at work and stress, he books in for a deep tissue massage to help his back muscles to loosen up.
ELBOW PAIN
Peter is retired and a keen gardener. He is right handed and a social smoker. He enjoys a variety of sports, including squash and golf.
He has noted pain to the outer aspect of his right elbow recently. It is also present at his left elbow, but to a much lesser extent. There is no obvious injury that he can think of that might have set this off.
It has now become so painful that his sleep has been badly affected. As a result, he feels exhausted and low. Painkillers, the use of an elbow brace and periodic rest have not been particularly helpful.
Peter is assessed in clinic where a history and detailed upper limb examination is undertaken. Lateral epicondylopathy (‘tennis elbow’) is suspected.
This is confirmed by means of a diagnostic ultrasound scan. A tear of the common extensor origin (one of the other possible diagnoses) is also excluded.
He is keen to get this problem resolved. Various options are discussed with him. He decides to go with the combined options of physiotherapy, acupuncture and a series of extracorporeal shockwave therapy (ESWT) sessions.
Lifestyle factors are also addressed, ensuring that he has an optimal diet and gets enough rest. Smoking can hinder tendon healing and he is advised to stop smoking. He is advised to speak to his GP regarding nicotine replacement therapy (NRT) and other strategies in order to optimise his chances of successfully quitting.
During physiotherapy, it is noted that Peter tends to grip his gardening tools (and steering wheel when driving) too tightly. There is also significant tightness in his shoulders and neck which are contributing to and manifesting as elbow pain. This vital information is communicated between doctor and physiotherapist.
After several weeks of treatment, his pain has settled significantly and his energy levels and mood have lifted too as a result of sleeping better. Peter is able to function well and return to participating in his favourite sports and gardening.
KNEE PAIN
Maria works in an office job. In her spare time, she enjoys distance running, doing so several times a week during her lunch break.
She has recently signed up for a marathon and has increased her running duration and frequency. She has noted increasing pain in her right knee that has not settled with either rest or icing it. This is so uncomfortable that it stops her from running and lingers on for several hours after the activity.
She attends the sports medicine clinic for consultation. A detailed history and clinical examination is carried out.
A diagnostic ultrasound scan of her right knee demonstrates abnormality to the iliotibial band, in keeping with iliotibial band friction syndrome (‘runner’s knee’).
Plain films (x-rays) of her knees and hips confirm that there is no significant degenerative change with the bones.
Maria is referred for physiotherapy and taping. She is also advised to stretch and use a foam roller regularly. She attends several physiotherapy sessions and notes an improvement in her pain intensity.
This improvement plateaus after several sessions and she returns to clinic for a planned review. The option of an ultrasound-guided corticosteroid and local anaesthetic injection (USGI) is discussed. This is intended to reduce pain and localised inflammation further, allowing her to progress with her rehabilitation and training.
Maria is given the opportunity to consider her options and decides to proceed with the USGI to the ITB. She is advised to rest for a few days afterwards, then gradually resume physiotherapy.
Ultimately, she is able to compete in the marathon and posts a decent time. She is advised to continue with the foam rolling, stretches and physiotherapy exercises to ensure that the problem does not recur. She is also advised to consult a podiatrist for a formal podiatry and gait assessment to see if her running style and footwear can be optimised.
Contact details:
(For all queries & appointments)
E: admin@sportsphysician.uk
T: 020 3488 9566 / 07788 78 75 74
F: 020 7691 9456
W: www.sportsphysician.uk
CLINICS: